Opioids have a high potential for abuse because of the way that they interact with your body. If you take opioid drugs for a long enough period of time, your body’s chemistry will adapt to the point where it needs them to survive. Ultimately, you could suffer serious withdrawal symptoms if you go even a few hours without your drug of choice. It’s fairly common to use suboxone to help safely wean yourself from opioid use disorder, but in some cases, you or your family member can actually become addicted to suboxone itself.
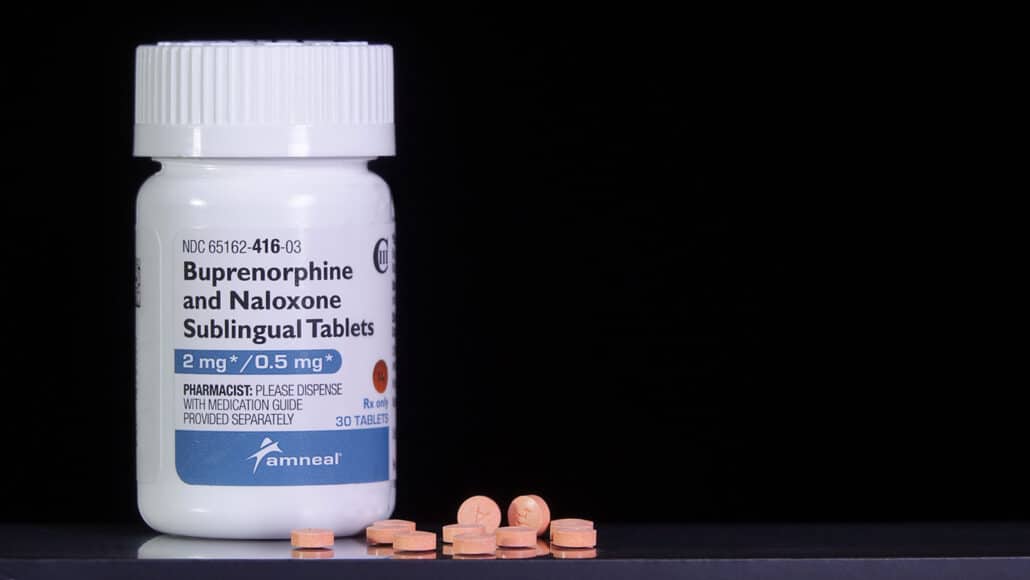
Table of Contents
- 1 What Is Suboxone?
- 2 Why Would Someone Take Suboxone?
- 3 How Long Do You Need to Take Suboxone?
- 4 What Are Some of the Differences Between Suboxone and Methadone?
- 5 What Are the Key Benefits of Suboxone Use?
- 6 What Are Some of the Potential Drawbacks to Suboxone Use?
- 7 Is Suboxone Addictive?
- 8 What Happens if You Miss a Dose?
- 9 Conclusion
What Is Suboxone?
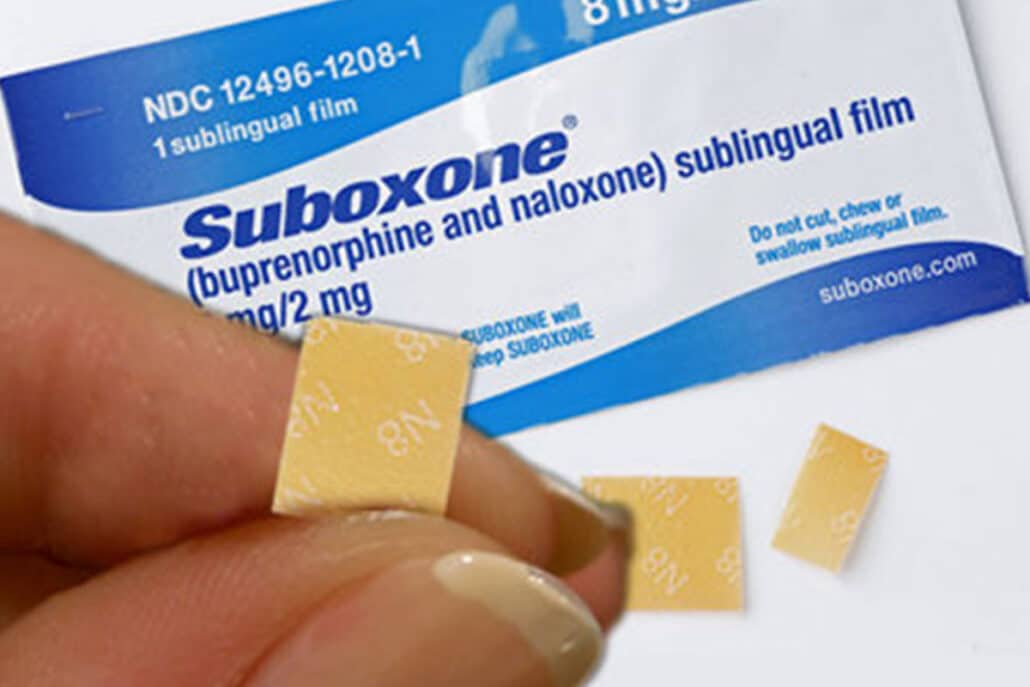
Suboxone is a combination of two medications known as buprenorphine/naloxone. This prescription drug is a drug approved by the Food and Drug Administration (FDA), which can be taken either in pill form or in the form of a strip that dissolves under your tongue. Although you generally need a prescription to take this substance, it may be possible to legally obtain and use it without a doctor’s permission or over the counter. However, you are strongly encouraged to consult with a medical professional or seek medical advice prior to taking it.
Does Suboxone is the same with methadone?
Suboxone is an opioid partial agonist. It binds to the opioid receptors in the brain but does not fully stimulate them like methadone usually does. Subxone may be less successful in managing cravings and opioid withdrawal symptoms in extreme cases of addiction due to its nature, which is only a partial opioid agonist.
Why Would Someone Take Suboxone?
Suboxone is designed to minimize or reduce the high that you feel whenever you take heroin, painkillers, pain medication, or anything else that has opioids in it. It can also help minimize the symptoms a person might feel during an initial withdrawal phase. You will generally see relief for about 24 hours after taking this medication, and it will typically remain in your system for about a week.
How Long Do You Need to Take Suboxone?
The answer to this question depends on your specific treatment needs. If you don’t have a history of addiction, it may be possible to take suboxone for just a few weeks or months before you are able to live a normal life without it. However, if you have a history of addiction, it may be necessary to take it for the rest of your life to guard against a future relapse.
What Are Some of the Differences Between Suboxone and Methadone?
While suboxone and methadone are both used to help patients manage their dependence on opioids, they do so in slightly different ways. For instance, methadone tends to induce a greater reaction in patients, which means that you can take it less often. Furthermore, the ingredients in methadone will generally have the same impact on a person each time that it is taken.
This means you can take it less often and at a consistent dose for months or years. Conversely, the effects of suboxone tend to peak as your body gets used to it, which may not be ideal for those who experience severe cravings or who need extra help getting past their addiction.
Another key difference between the two substance uses is that methadone can be taken at most medical facilities while suboxone must be taken at a formal clinic. In some cases, it may even be possible to take methadone at home without a doctor’s supervision. Of course, this generally only happens after a patient has gained the trust of the medical professional prescribing it, which can take months or years to occur.
It’s not uncommon for individuals to take both substances as their needs change over time. The type of medication that you take may also depend on how your body reacts to them. It’s important to note that you shouldn’t take both at the same time, as it could cause a negative interaction. At a minimum, you’ll need to wait until one medication has cleared your system before taking the other.
What Are the Key Benefits of Suboxone Use?
One of the primary benefits of using suboxone is that you have a relatively low risk of abusing it. This is partially because you can change the dosage as your desire for opioids increases or decreases. Those who use suboxone for a long period of time usually start with a higher dose and then gradually reduce it over a period of weeks, months, or years.
Those who opt to use suboxone for the rest of their lives typically take a smaller dose that won’t cause harsh adverse effects of opioids. In many cases, patients who use it for long periods of time do so because they can’t stop using it altogether without experiencing symptoms and p that are severe enough to interrupt their lives.
What Are Some of the Potential Drawbacks to Suboxone Use?
The Substance Abuse and Mental Health Services Administration (SAMHSA) said that These are common side effects of suboxone usage. It can also result in increased anxiety or feelings of depression. Therefore, if you already experience symptoms of anxiety or depression, it’s critical that you let your doctor know this before taking this substance. He or she may be able to adjust your dosage or take other steps to ensure that your treatment plan is administered in a safe and effective manner.
It’s also common for people who take this substance to experience insomnia, sudden drowsiness, or both. Ideally, you will not drive a car or operate other heavy machinery until you know that suboxone will not have an impact on your sleep cycle. Suppose suboxone does have a negative impact on your sleep cycle. In that case, it may be possible to ask for accommodations from your employer to ensure your safety and the safety of other employees.
Changes in mood or overall personality may also occur if you take suboxone. In some cases, irritability, anger or hostility may simply be a response to the stress of withdrawing from something you have depended on for a significant time. However, it’s also possible that the suboxone itself is responsible for mood swings, trouble concentrating, or short-term memory loss. Your doctor may be able to provide more insight into what you are experiencing and provide strategies to help you cope with these issues.

Is Suboxone Addictive?
For many people, suboxone itself is not addictive. However, this doesn’t mean that you can’t become dependent on it or that there is no risk of abuse. It is worth noting that this substance is much less likely to be abused than methadone, which is something that you might want to consider when choosing a medication. If you feel as if you are becoming dependent on suboxone, it may be possible to reduce your dose or use other medications to avoid secondary problems.
What Happens if You Miss a Dose?
As with most other medications, suboxone works best when you follow the dosage schedule provided by your doctor or another medical professional. As a general rule, you can take a dose as soon as you remember to do so, as long as it’s not too close to your next one. Otherwise, simply wait until you are supposed to take your next pill or strip.
If you do miss a dose, do not try to make up for it by taking two pills or strips later in the day. Doing so may increase your risk of overdosing, which can result in serious and long-term healthcare problems, and it’s possible that you can die from an opioid overdose if you are not treated quickly enough. Signs of a potential overdose include trouble breathing or passing out with little or no warning.
Conclusion
The first step toward overcoming an opioid addiction is admitting that you need help to do so. At Long Island Interventions, as a healthcare provider, we have a variety of treatment options like medication-assisted treatment and behavioral therapy targeted to meet your needs today due to medical conditions involving drug abuse, opioid dependence, and programs capable of evolving as your needs change. You can call us or send a message through our site to learn more about our services or begin your drug addiction treatment program today.

