Have you ever thought of drinking alcohol while under medication due to like high blood pressure, liver damage, or chest pain? Can you drink a red wine with penicillin? Like even just a tiny amount of alcohol?
Alcohol consumption can lead to unpleasant side effects that aren’t always easy to manage. While everyone should be careful on alcohol use, the effects of this consumption become even more dangerous to your immune system when you combine this substance with penicillin or other antibiotics. It can be challenging to predict what these effects will be. If any medication has been prescribed to you, you must read the product label or patient information pamphlet to identify how the medicine should be taken. If not, then what a brave one you are.
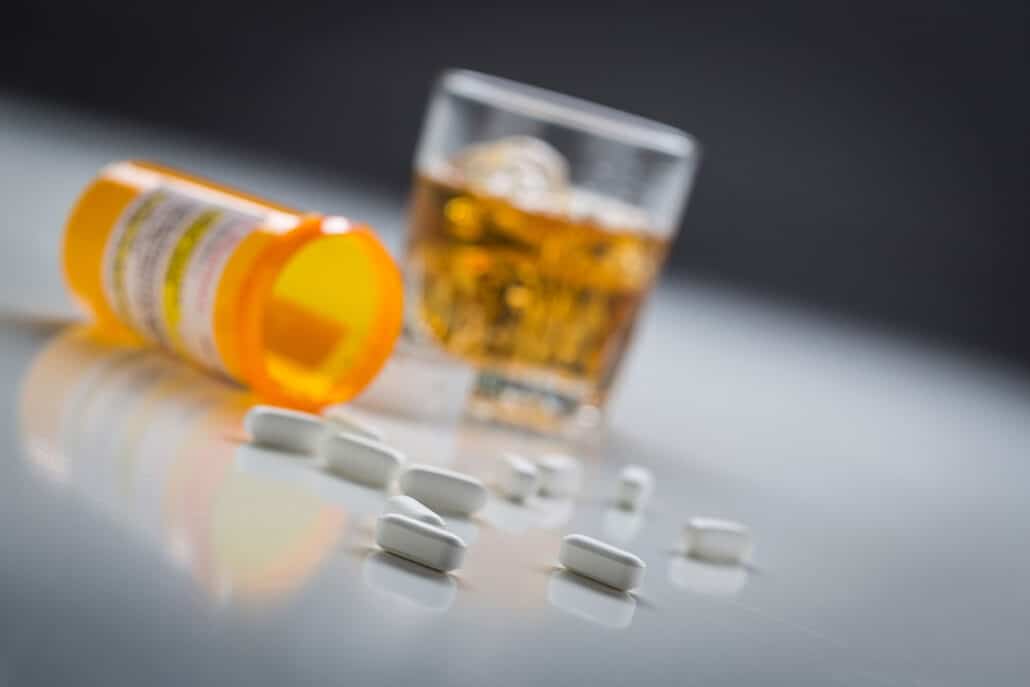
Table of Contents
Why You Should Avoid Mixing Alcohol with Antibiotics like Penicillin
Even though most antibiotics are outfitted with packaging that warns people not to drink alcoholic beverages with antibiotics, it’s commonly misunderstood that drinking alcohol with medications is safe. In reality, alcohol dampens the effects of antibiotics – this medication interaction may lead to many adverse side effects and affect the body’s ability.
Once your body breaks down alcohol, a substance known as acetaldehyde is produced, which may lead to nausea, any individual taking antibiotics to relieve stomach pain or digestive problems could experience worsening symptoms after combining alcohol and antibiotics.
This combination also creates issues with a person’s concentration, coordination, and cognitive function. If you suffer from a bacterial infection, drinking alcohol can disrupt the hydration and sleep processes that your body requires to recover effectively.
What Are Antibiotics?
Antibiotics are potent medications that can slow down or destroy bacteria growth that’s why medical advice is a must. This type of medication doesn’t attack infections caused by viruses like the flu or a cold. Instead, antibiotics attack infections from bacterial diseases.
These medications are designed to prevent antibodies from reproducing or killing invading bacteria. Even though the white blood cells in your body are meant to eradicate harmful bacteria, these cells might not be strong enough if the amount of harmful bacteria is too high. The types of conditions that antibiotics can properly treat include:
- Urinary tract infections
- Ear infections
- Strep throat
- Bacterial pneumonia
- Sexually transmitted diseases
- Sepsis
- Skin infections like acne
The majority of antibiotics are safe to use when taken as prescribed. However, side effects are always possible, including everything from an upset stomach to diarrhea and nausea. These effects can be strengthened if the antibiotics are taken alongside alcohol. In this scenario, some additional side effects you might experience include:
- Drowsiness
- Vomiting
- Dizziness
- Headaches
- Seizures

What Are The Common Antibiotics?
After learning the basic information about antibiotics, let’s delve into the different types of antibiotics.
Antibiotics are readily available and go by a number of distinct brand names. Antibiotics are often categorized according to their modes of action. Antibiotics are only effective against specific kinds of parasites or bacteria. For this reason, various infections are treated with different antibiotics. The primary classes of antibiotics consist of:
- Penicillins – for example, phenoxymethylpenicillin, flucloxacillin, and amoxicillin.
- Cephalosporins – for example, cefaclor, cefadroxil and cefalexin.
- Tetracyclines – for example, tetracycline, doxycycline, and lymecycline.
- Aminoglycosides – for example, gentamicin and tobramycin.
- Macrolides – for example, erythromycin, azithromycin, and clarithromycin.
- Clindamycin.
- Sulfonamides and trimethoprim – for example, co-trimoxazole.
- Metronidazole and tinidazole.
- Quinolones – for example, ciprofloxacin, levofloxacin, and norfloxacin.
- Nitrofurantoin – used for urinary infections.
So, what are now the common antibiotics?
- Gentamicin (also known as tobramycin, neomycin, amikacin, and streptomycin). It is usually used in hospitals to treat severe illnesses like sepsis, as this can have major adverse effects, such as renal damage and hearing loss. Although they are often administered by injection, in some instances, drops may be used to treat ear or ocular infections.
- Ertapenem (meropenem, imipenem, etc.). This one is frequently used for infections of the abdomen and gynecological system, community-acquired pneumonia, and diabetic patients’ foot infections affecting the skin and soft tissues.
- Cephalexin (also cefuroxime, ceftriaxone, ceftazidime). This is a broad-spectrum antibiotic. It is said that different ones are used for the treatment of sepsis, pneumonia, meningitis, and biliary and urinary tract infections.
- Levofloxacine. This is used to treat infections of the joints and bones (including osteomyelitis), pelvic inflammatory disease, infections of the abdomen, abscesses, and acne. When other antibiotics have failed to treat tooth infections, it is also utilized in those situations.
- Erythromycin, also known as azithromycin and clarithromycin. Used for dental abscesses, rosacea and acne, pneumonia, and some STDs (sexually transmitted infections). They are used to treat bacterial strains resistant to penicillin or as a substitute for those who are allergic to the antibiotic.
- Ciprofloxacin, also known as moxifloxacin and levofloxacin. It is effective against infections of the respiratory tract, the gastrointestinal tract (including typhoid fever), the bones and joints, gonorrhea, sepsis, and respiratory tract infections (but not pneumococcal pneumonia). However, due to the possibility of severe side effects, these antibiotics are no longer prescribed on a regular basis.
- Benzylpenicillin, also known as ticarcillin, piperacillin, and amoxicillin. It is being used as a preventative measure against rheumatic fever, for ear and skin infections, meningitis, pneumonia, and Strep A throat.
- Tetracycline is commonly known as minocycline and doxycycline. This one is used to treat various STDs (including syphilis, gonorrhea, and chlamydia) and severe acne and is additionally used for plague, brucellosis, and cholera.
- Trimethoprim-sulfamethoxazole (also known as “Septrin”). In this class, antibiotics work well against a wide range of illnesses. They function by stopping bacteria from making a type of folic acid that is necessary for their growth and multiplication.
- Methanidazole. When it comes to anaerobic bacteria and protozoa, this antibiotic is highly active. Indicated for bacterial vaginosis, rosacea, pelvic inflammatory illness, and dental abscess/gum disease.
These illustrate the applications of various antibiotics (in different groups): Bacitracin, Chloramphenicol, Ethambutol, Fusidic acid, Isoniazid, Mupirocin, Nitrofurantoin, Pyrazinamide, Rifampicin, Trimethoprim, Vancomycin and Linezolid.
What Is Penicillin?
Penicillin is the name used for a group of drugs that are designed to attack many different types of bacteria. These antibacterial drugs are derived from the penicillium fungi and can be taken orally or through an injection.
Today, people use penicillin to treat numerous diseases and infections, extending to ear, skin, dental, and respiratory tract infections.
Medications within the penicillin class indirectly burst bacterial cell walls, which helps to kill harmful bacteria. This process works by focusing on the structural elements of bacterial cells known as peptidoglycans, which form mesh-like structures in bacterial cells.
Penicillin directly blocks the proteins that link peptidoglycans together, which ensures that the bacterium cannot close off holes that develop. Water will then flow through these holes, which results in the bacterium bursting. While penicillin is a highly effective medication, this drug’s potency is why it shouldn’t be combined with alcohol.
Effects of Drinking Alcohol with Penicillin
There’s no direct drug interaction found between alcohol and penicillin. However, taking these two substances together can create problems for people suffering from an infection. When consumed, alcohol reduces your immune function, which can result in the side effects of penicillin worsening and even other antibiotic interactions.
A few side effects that can be more severe after combining alcohol and penicillin include an upset stomach, nausea, and diarrhea. Make sure that you stay well hydrated to keep these effects at bay.
If you combine penicillin with alcohol, the amount of time this drug remains in the body differs with each individual. The half-life of the drug is upwards of 45 minutes for healthy individuals.
If you suffer from liver or kidney impairment, the half-life of penicillin can be as long as 30 hours. Because of this drug’s half-life will leave a healthy person’s body after 12 hours or so. It can take several days to leave the body for those with liver or kidney impairment.
Avoid Drinking Alcohol with Penicillin and Other Antibiotics
Along with worsening the medication’s side effects, taking alcohol with penicillin may also disrupt the healing process for your infection or disease. If you’re currently suffering from alcoholism, not drinking until penicillin has left your body might seem too challenging for you. If you find yourself in this situation, you should get in touch with a treatment healthcare provider or healthcare professional to start gaining control of your life once more.
Even though the effects aren’t always has a severe reaction, it’s never a good idea to drink alcohol with penicillin. If you’ve been prescribed penicillin to treat a recent infection or disease, your recovery process will be aided by not drinking alcohol until your treatment ends. Call Long Island Interventions today for more information on addiction and the most commonly used treatment options.
FAQ
Can you drink alcohol while taking Penicillin?
What not to take with penicillin?
Published on: 2022-10-31
Updated on: 2024-06-21

